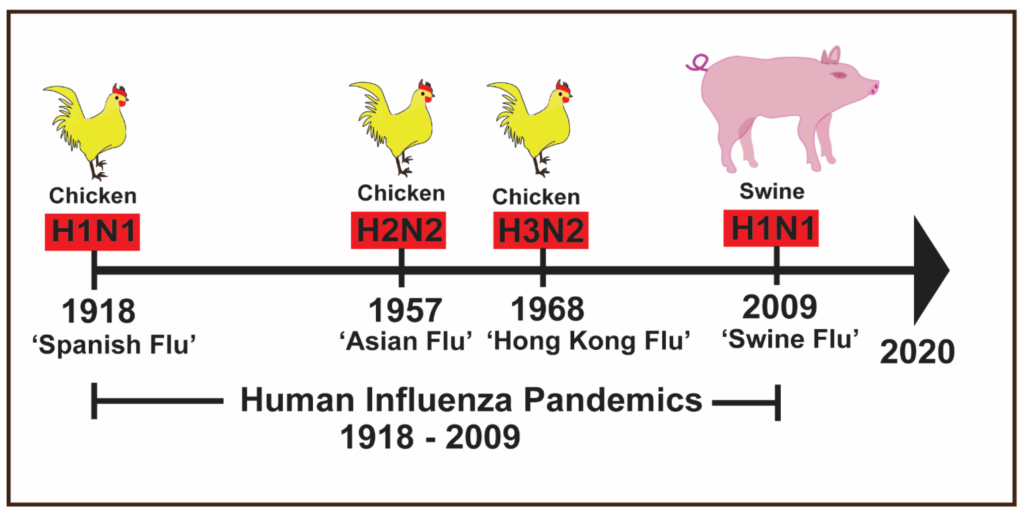
H2N2 virus, also known as the Asian flu virus, is a subtype of the influenza A virus that caused a global pandemic in 1957-1958. The virus was first identified in Asia in early 1957 and quickly spread to other parts of the world, including the United States, where it caused widespread illness and death.
The symptoms of H2N2 virus are similar to those of other flu viruses and can include fever, cough, sore throat, body aches, and fatigue. The virus is transmitted from person to person through respiratory droplets produced when an infected person coughs or sneezes.

In the years following the 1957-1958 pandemic, the H2N2 virus underwent antigenic shift, a process by which the virus undergoes major genetic changes that can result in the emergence of a new subtype. As a result, H2N2 is no longer a circulating strain of influenza A, and most people today have no immunity to it.

What is the full form of H2N2?
The letters and numbers in the term indicate the type of hemagglutinin (H) and neuraminidase (N) proteins present on the surface of the virus. The H2N2 virus contains the H2 type of hemagglutinin protein and the N2 type of neuraminidase protein. Therefore, there is no full form of “H2N2” as it is a scientific naming convention for a specific strain of the influenza A virus.
What is Hemagglutinin in layman term?
In layman’s terms, hemagglutinin is a protein found on the surface of the influenza virus that helps the virus bind to and infect host cells. The name “hemagglutinin” comes from its ability to cause red blood cells to clump together, or agglutinate, which was its original discovery method. Hemagglutinin is an important target for the body’s immune system to recognize and produce antibodies against, as it plays a key role in the entry of the influenza virus into cells. Influenza viruses have different subtypes of hemagglutinin, designated by numbers, such as H1N1 or H3N2, which can indicate differences in the virus’s ability to spread and cause disease.
What is Neuraminidase in layman term?
In layman’s terms, neuraminidase is an enzyme found on the surface of the influenza virus that helps the virus to release itself from infected cells, so that it can spread to other cells and cause more infection. The name “neuraminidase” comes from its ability to cleave or break down sialic acid molecules that are found on the surface of host cells and the virus itself. By cleaving these molecules, neuraminidase enables the virus to detach from the infected cell and move on to infect other cells.
Neuraminidase is also an important target for antiviral medications, such as oseltamivir and zanamivir, which work by blocking the activity of this enzyme and preventing the release of new viral particles. Influenza viruses have different subtypes of neuraminidase, designated by numbers, such as N1 or N2, which can indicate differences in the virus’s ability to spread and cause disease.
What is the difference between H1N1 and H2N2?
H1N1 and H2N2 are two different subtypes of the influenza A virus, each with a unique combination of hemagglutinin (H) and neuraminidase (N) proteins on their surface. Here are some of the key differences between H1N1 and H2N2:
- Historical Context: H1N1 was responsible for the 1918 flu pandemic, also known as the Spanish flu, which was one of the deadliest pandemics in history. H2N2 caused the Asian flu pandemic in 1957-1958.
- Hemagglutinin Protein: H1N1 has the H1 type of hemagglutinin protein, while H2N2 has the H2 type of hemagglutinin protein. The H1 protein is different from the H2 protein, and these differences can affect the way the virus interacts with host cells and how the immune system responds to the virus.
- Neuraminidase Protein: H1N1 has the N1 type of neuraminidase protein, while H2N2 has the N2 type of neuraminidase protein. Like the hemagglutinin protein, the neuraminidase protein is also different between the two subtypes, which can affect the virus’s ability to spread and cause disease.
- Immunity: Because H1N1 and H2N2 are different subtypes of influenza A virus, people who were exposed to or vaccinated against one subtype may not have immunity to the other. This means that if either of these viruses were to re-emerge in the future, they could cause a significant outbreak or pandemic, particularly if they underwent antigenic drift or shift, a process by which the virus evolves and develops new variants that may not be recognized by the immune system.